Deep Neck Space Infections
Red flags
The airway disaster triad (see below) alerts you to either epiglottitis or deep neck space infections (DNSI)
Symptoms of neck stiffness and fever may be due to meningitis and therefore this must be included in your differential diagnosis
DNSI may progress rapidly to stridor, indicating imminent airway obstruction.
Do not be fooled by a relatively well-looking patient – rapid decompensation can occur.
ENTSHO.COM IMPENDING AIRWAY DISASTER TRIAD
Rapid onset aphagia or severe dysphagia, frequently associated with a severe sore throat
Rapid onset laryngeal voice change: hoarse, croaky, husky or no voice
Systemically very unwell: pyrexia, tachycardia, tachypnoea
There may be associated trismus or torticollis. Beware of any patient who develops these signs after admission: situations deteriorate rapidly. In the presence of neck trauma, any of the above should be taken very seriously. Stridor is a late sign of airway compromise.
Why is this important?
DNSI may need surgical drainage under general anaesthetic and admission to critical care.
If left, DNSI will cause airway obstruction. They can track down into the mediastinum, requiring cardiothoracic surgical support.
When to involve the ENT registrar
Immediately: DNSI are an airway emergency.
Patients with deep space neck infections can rapidly develop airway obstruction (particularly children due to their narrow airway). Always inform your senior when you are unsure of the diagnosis, as the differential includes other emergencies like epiglottitis or meningitis.
Who to admit
Admit all patients you suspect to have a DNSI or who have airway disaster triad symptoms.
Assessment and recognition
History may indicate a preceding upper respiratory tract infection, ingested foreign body, peritonsillar abscess or dental abscess.
Cardinal symptoms include the airway disaster triad:
Severe sore throat with dys- or aphagia
Laryngeal voice change eg hoarseness or voice loss
Systemically unwell eg fever and dehydration
Neck pain and stiffness
In children: drooling; agitation; off feeds
The differential diagnosis includes both medical and surgical emergencies and therefore one must have a high index of suspicion for these.
Examination findings may include:
Stridor
Head tilt to one side
Trismus
Cervical lymphadenopathy
Unilateral smooth swelling of the posterior pharyngeal wall (the abscess is contained to one side of the midline because of the median raphe of the buccopharyngeal fascia).
Signs of sepsis
Drooling or agitation
There may be concurrent tonsillitis, pertonsillitis, pharyngitis and other upper respiratory infection such as otitis media
NOTE - The general prohibition on instrumenting the mouth or performing nasendoscopy in patients with an airway problem prevents over-zealous and uncontrolled instrumentation of the base of tongue/larynx by first responders. Controlled, careful and minimal instrumentation by trained personnel is lower risk.
Immediate and overnight Management
Bear in mind the Sepsis Resuscitation Bundle when managing septic patients.
Follow the ABCDE algorithm. Instigate the following procedures and investigations:
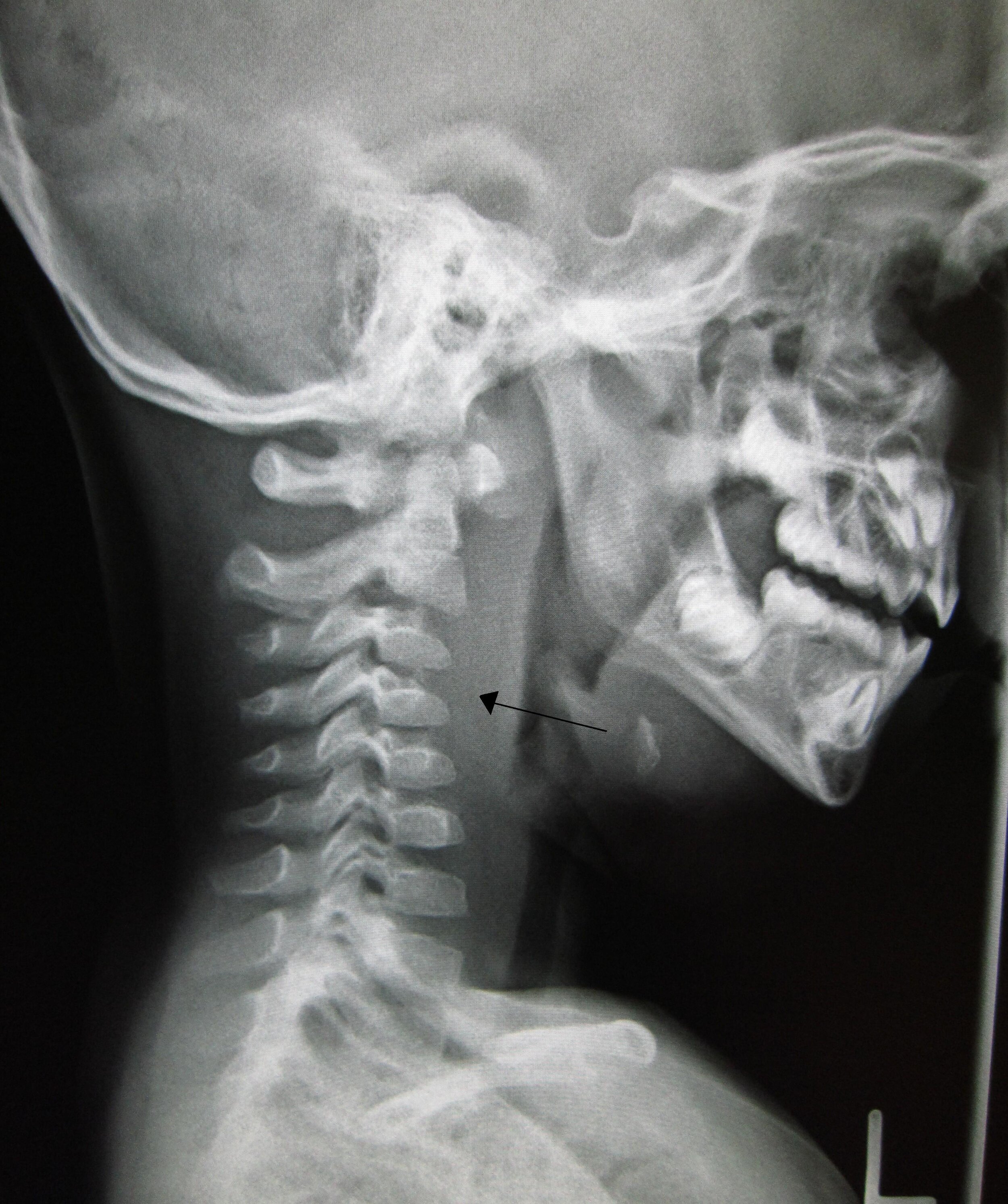
Lateral soft tissue neck X-ray showing ‘straight neck sign’ (loss of lordosis due to spasm). The arrow indicates widening of prevertebral soft tissue in a child
With thanks to James Heilman MD, Wikimedia Commons
IV access + FBC (neutrophilia), CRP, U&Es, blood cultures (usually negative)
Keep NBM until senior review and initiate IV fluids
Initiate broad spectrum IV antibiotics and analgesia
Humified oxygen and back-to-back saline nebulisers
Consider stat or PRN adrenaline nebulisers
Flexible nasendoscopy performed by a competent endoscopist (trained SHO or ANP; registrar) viewing the oropharynx and larynx from just beyond the soft palate; do not advance too far as instrumenting the larynx can precipitate respiratory arrest
Lateral soft tissue neck X-Ray if safe. This may show the ‘straight neck sign’ (Figure 1) whereby the cervical vertebral column has lost its natural lordosis. There may also be widening of the pre vertebral soft tissue shadow. This may also manifest as a pushing forward of the airway. Very rarely an air-fluid level may be seen in the prevertebral area.
CT scan (ideally with contrast) will confirm the diagnosis and the extent/anatomical relations of the abscess. Make sure you have a secure airway (elective intubation or anaesthetic escort).
Nurse upright (more than 45 degrees)
Further management
The standard management of DNSI includes drainage but a some small abscesses will resolve with conservative treatment. Management will depend on the underlying cause, as well as the location of the abscess, for example:
Removal of any causative foreign body that has caused a retropharyngeal abscess
Drainage of any peritonsillar abscess +/- immediate 'hot' tonsillectomy (rare) for a parapharyngeal abscess
Drainage of dental abscess for Ludwig's angina (floor of mouth abscess)
One study found that of 162 paediatric patients with retropharyngeal abscess, 126 required surgery initially and, of the 36 patients initially treated conservatively with high-dose antibiotics, 17 required surgery (1).
Drainage can be done through the mouth or through the neck (depending on the type of abscess): consult senior colleagues.
Any sign of airway compromise may require awake intubation and/or local anaesthetic tracheostomy which could be performed at the time of drainage.
An associated phenomenon is Lemierre's syndrome where a DNSI is associated with an infective thrombophlebitis of the ipsilateral internal jugular vein. The causative organism is frequently Fusobacterium necrophorum; there may also be synergistic bacterial infection. It is mandatory to get a haematology opinion on anticoagulation.
Reference
Page NC, Bauer EM, Lieu JE; Clinical features and treatment of retropharyngeal abscess in children. Otolaryngol Head Neck Surg. 2008 Mar;138(3):300-6.
Page last reviewed: 12 October 2022