Periorbital Cellulitis
Red flags
Compromised vision
Symptoms or signs of meningism
Sepsis
Why is this important?
Permanent loss of vision can occur if periorbital cellulitis is not treated promptly. If the optic nerve is at risk and decompression is not achieved within hours, irreversible damage may occur.
Intracranial complications may occur concomitantly, e.g. meningitis, cavernous sinus thrombosis
When to involve the ENT Registrar
Urgently: Signs of severe disease with eye compromise (chemosis, proptosis, loss of colour vision etc.) - see below
Soon: Signs of moderate disease eg pre-septal cellulitis
Care is normally shared between ophthalmology and ENT (+/- paediatrics), with involvement of neurosurgery if indicated
Who to admit
Always err on the side of caution. Many units would admit patients with any periorbital swelling for a minimum of overnight treatment and observation. Patients with significant swelling or any red flags should be urgently treated, admitted, considered for imaging and kept nil-by-mouth.
Assessment and recognition
Pathophysiology
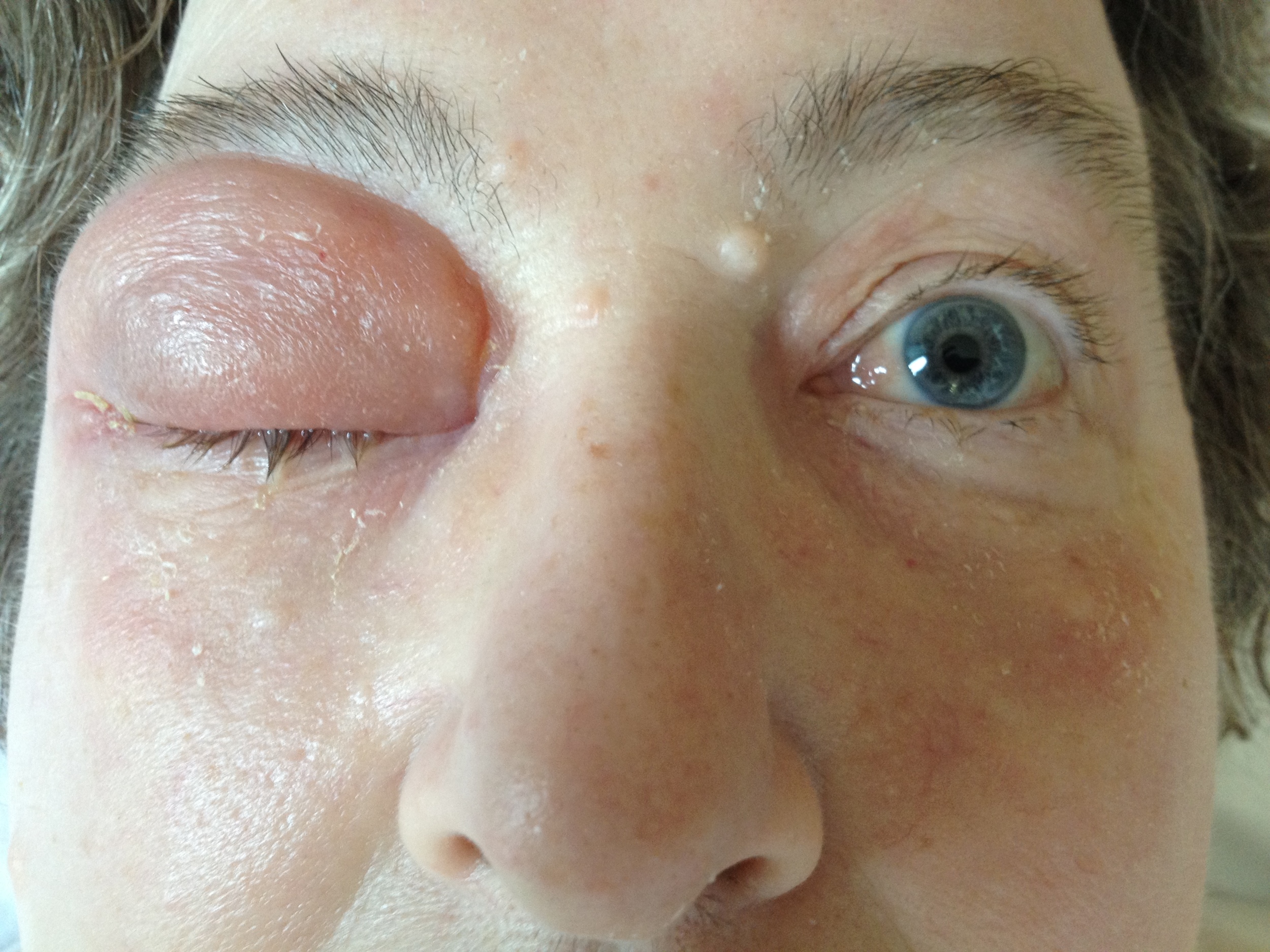
Photo: right pre-septal (Chandler I) cellulitis. Note how the erythema is clearly confined to the eye lid.
Arising from insect bites or periorbital trauma (including ENT/maxillofacial/ophthalmology procedures): likely to result in pre-septal cellulitis
Arising from sinusitis; fronto-ethmoidal sinus pathology is the usual culprit: more likely to result in orbital cellulitis or abscess
Chandler’s classification gives five different types of periorbital infection (they are not "stages"):
I. Pre-septal cellulitis - cellulitis confined to the eyelids i.e. anterior to the orbital septum
II. Orbital cellulitis without abscess - cellulitis involving the orbit including post-septal tissues
III. Orbital cellulitis with subperiosteal abscess - cellulitis with abscess confined to the orbital periosteum. The abscess is most common based medially on the lamina papyracea but can be elsewhere
IV. Intra-orbital abscess - an abscess in the intraconal compartment (behind the globe between the extra-ocular muscles)
V. Cavernous sinus thrombosis - bilateral periorbital swelling with proptosis, ophthalmoplegia and neurological signs. This has a high mortality and is thankfully rare.
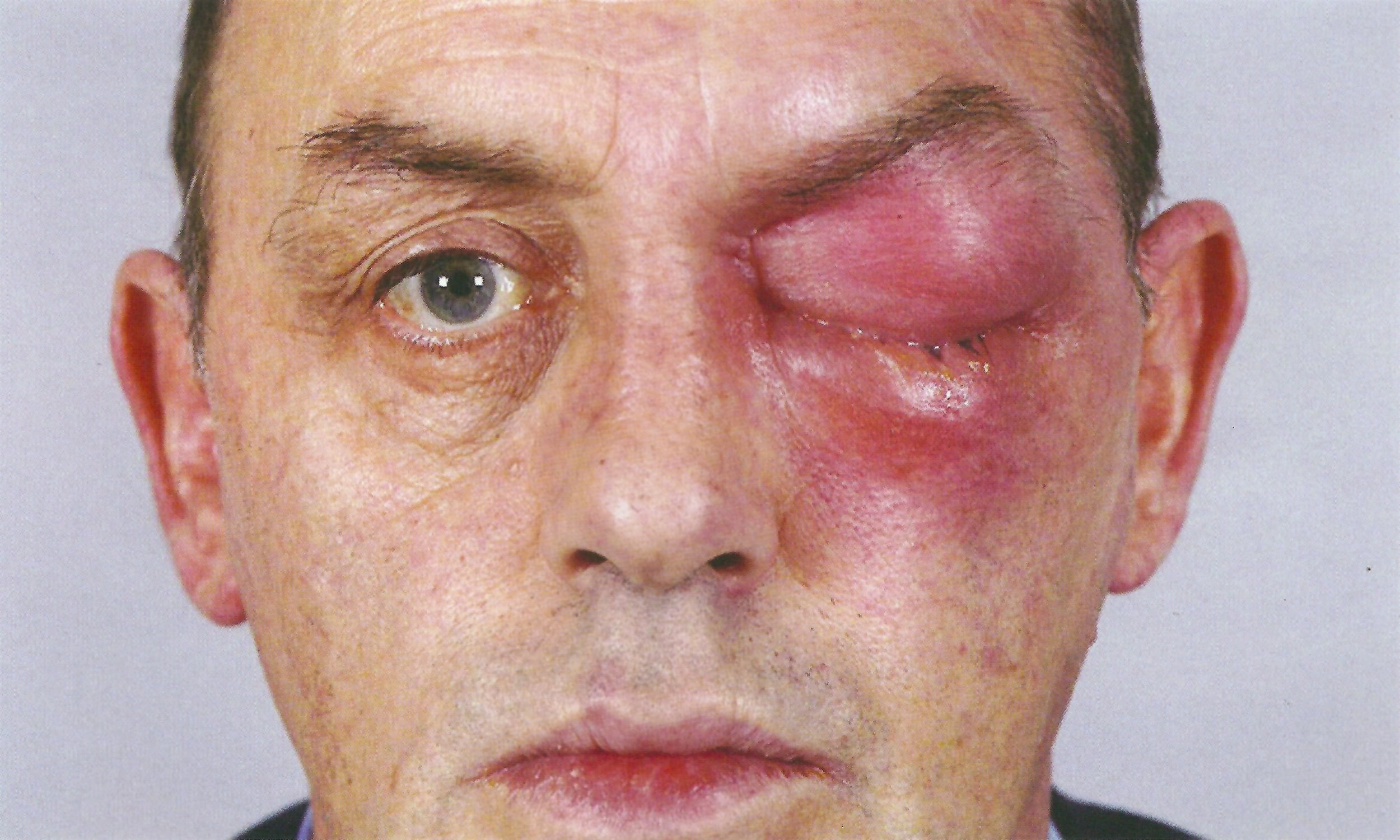
Photo: left post-septal (Chandler II) or orbital cellulitis. Note how the erythema involves the brow, orbit and maxilla.
The three crucial components of the examination are the eye, the nose and neurology.
Eye examination
Whilst the ophthalmologist will provide a more detailed examination, the ENT doctor should have performed a basic eye exam. It is essential to look for any signs of eye compromise. Check for:
Opthalmoplegia/diplopia
Pain on eye movements
Proptosis - look from above the brow
Visual acuity - use a Snellen chart
Colour vision and discrimination - loss of colour vision is a worrying sign and red reportedly goes first; use an Ishihara chart for red/green discrimination
Fundoscopy - engorgement of retinal veins
Nose examination
Nasendoscopy is essential: note the appearance of the nasal mucosa in general and middle meatus area specifically
Any discharge should be swabbed and sent for culture
Neurological examination
A general neurological and cranial nerve examination is essential
Investigations
Send bloods for FBC, CRP, U&E, blood cultures, ABG/lactate (if septic).
A CT orbits/sinuses with contrast is the gold standard in the emergency setting. Imaging should performed urgently if there are any signs of eye compromise (above), if it is not possible to assess the eye due to severe swelling, or if the patient fails to respond to around 24 hours of medical treatment. If a patient has no signs of eye compromise they may be admitted on medical treatment without further investigation, but discuss with your senior if you are unsure.
Immediate and overnight management
Bear in mind the Sepsis Resuscitation Bundle when managing septic patients.
Non-surgical management
Broad spectrum IV antibiotics - consult your local microbiology guidance
Nasal decongestants
Steroid nasal drops
Nasal douches
Supportive: IV fluids, analgesia
Further management
You will need senior input for the following:
Surgical drainage of intraorbital collection:
External-approach drainage (via Lynch-Howarth incision if medial). The most reliable approach in a compromised eye or where access is challenging (e.g. young children).
Endoscopic approach via an ethmoidectomy.
Further imaging may be indicated if the patient fails to progress on medical treatment for 24-36 hours, or if a procedure fails to result in significant improvement.
Page last reviewed: 1 December 2022